Figure 1
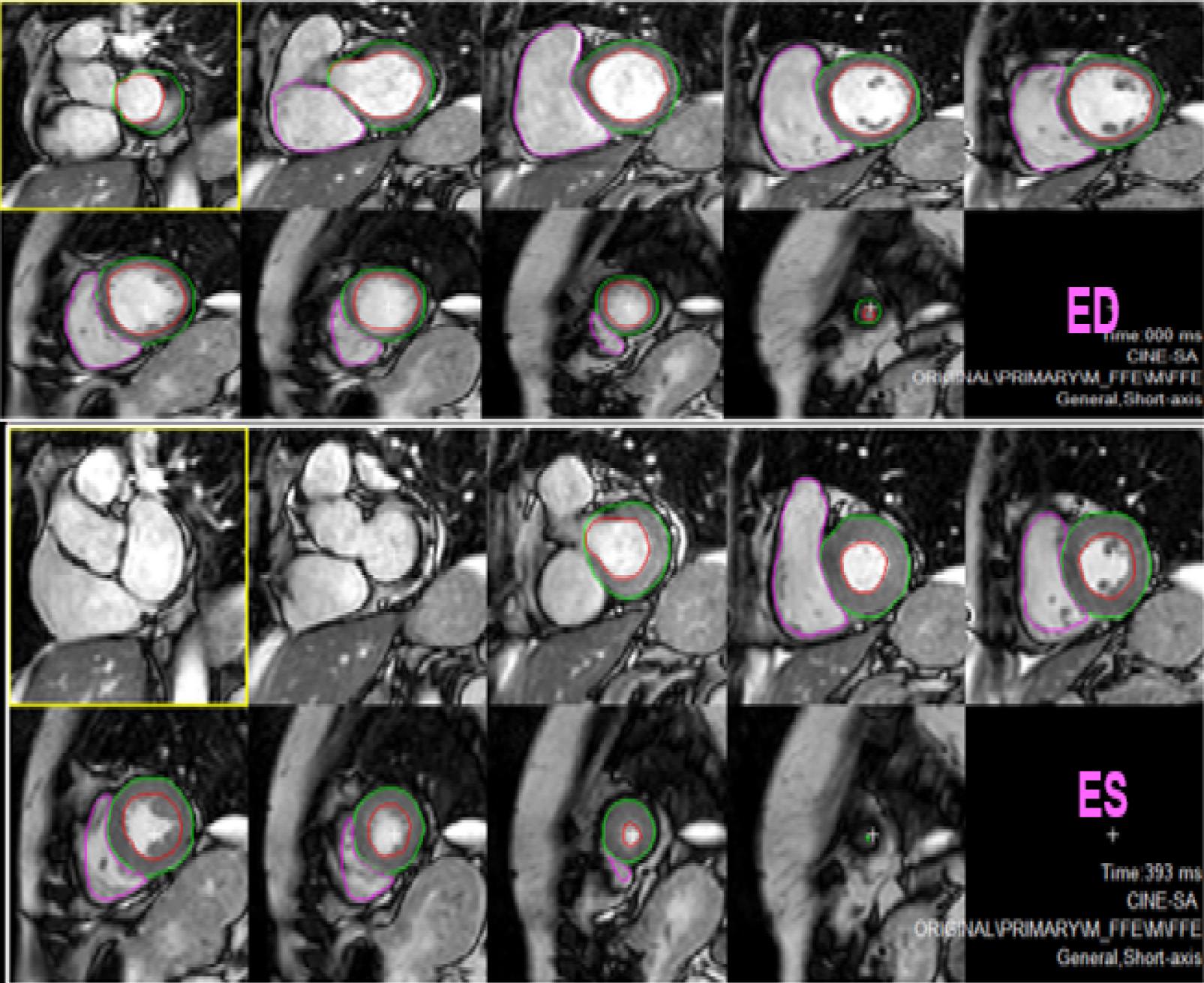
Figure 2
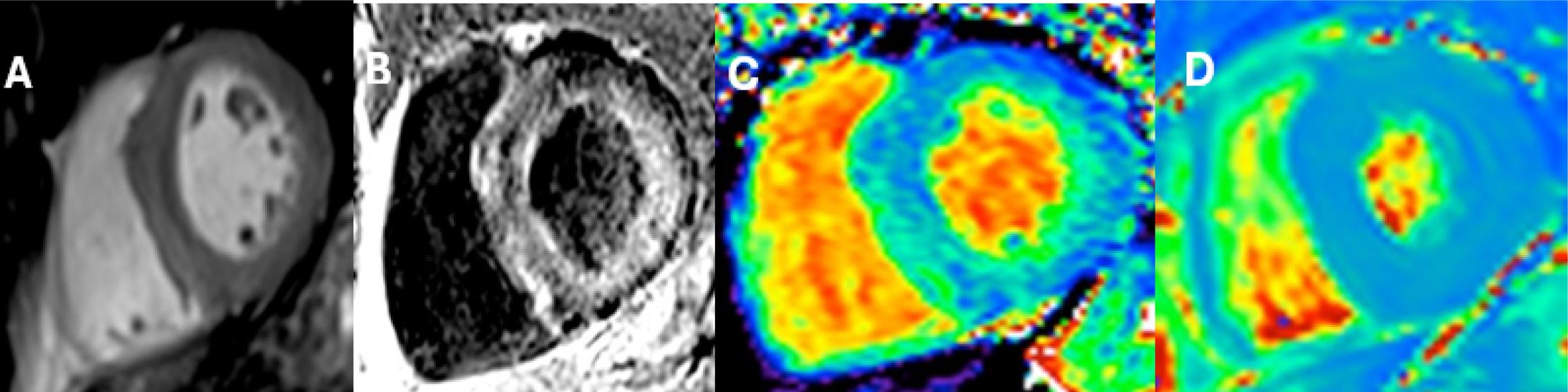
Figure 3
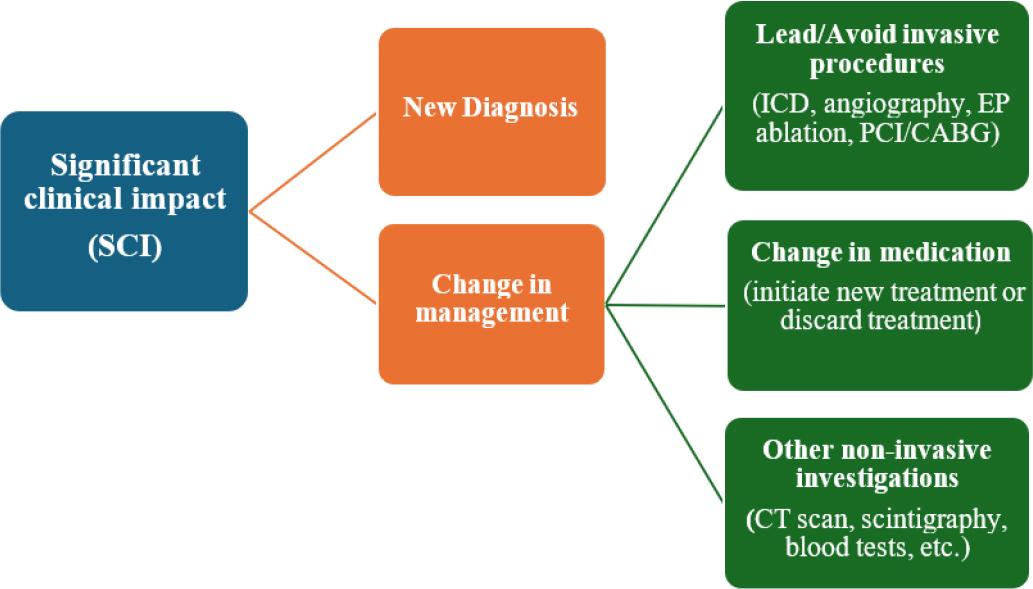
Figure 4
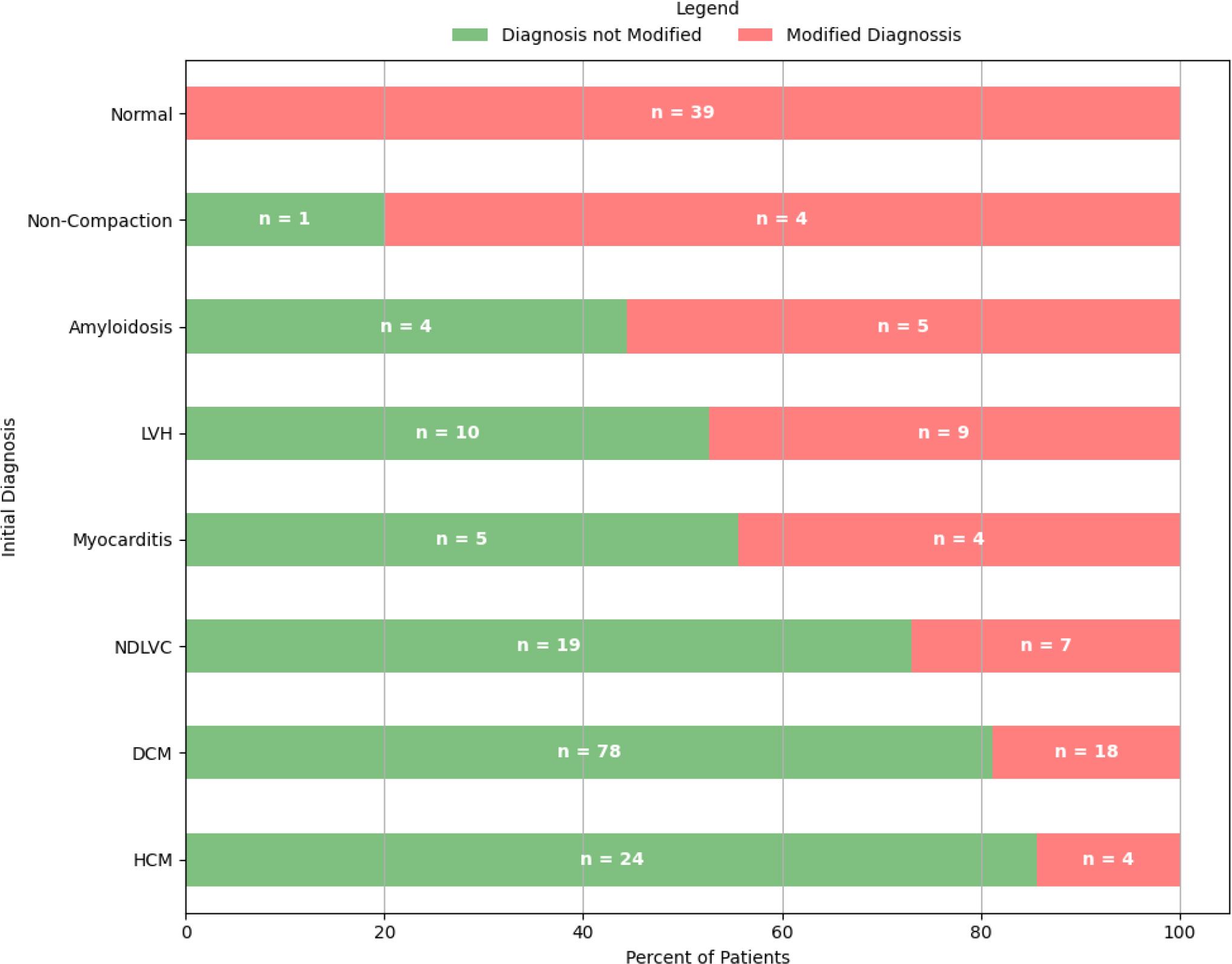
Figure 5
Comparison of CMR’s significant clinical impact in current studies
| Study | Study period | Study patient | n | Change in diagnostic (%) | Change in management (%) |
|---|---|---|---|---|---|
| Bruder O et al. [28] | 2007-2009 | euro CMR registry (German pilot) | 11, 040 | 16.4% | 61.8% |
| Bruder O et al. [20] | 2006-2012 | SCMR registry | 27,301 | 8.7 % | 61 % |
| Roifman et al. [19] | 2013-2019 | Patients with HF indications from the SCMR registry | 3,837 | 49% | - |
| Abbasi et al. [21] | 2013 | Patient with LVEF < 50%. | 150 | 52% | 65% |
| Lin et al. [3] | 2004-2017 | Patients Undergoing Cardiac Transplantation | 338 | 23 (7%) | |
| Kangala et al. [22] | 2017 | Patient with HFpEF | 154 | 27% | |
| Witek et al. [29] | 2008-2017 | Patient with HF of unknown etiology | 243 | 38. 7% | 16.9% |
| Onciul et al. [30] | 2018-2020 | Patient referred for stress CMR | 120 | 15.85% |
CMR criteria for the majority of cardiomyopathy diagnoses
| Indication | Structural Features (cine-SSFP) | LGE | Native T1 | ECV | T2 |
|---|---|---|---|---|---|
| DCM | -LV dilatation and disfunction - diffuse regional wall motion abnormalities - +/_RV dilatation and disfunction | - typical mid-wall pattern | -slightly diffuse increased | -slightly increased | - slightly increased, especially in inflammatory etiologies |
| NDLVC | -no LV dilatation with LV disfunction -normal LV systolic function with + LGE | -nonischemic pattern | -normal -slightly increased | -normal -slightly increased | -can be increased in inflammatory etiologies |
| Myocarditis | -none -regional wall motion abnormalities -global LV dysfunction -pericardial effusion | -patchy subepicardial pattern | -increased in the oedema zone | -increased in the oedema zone | -regional or global increased |
| HCM | -hypertrophy (≥15 mm LV wall thickness): symmetrical, asymmetric, apical - other anomalies: LV crypts, papillar hypertrophy, SAM | -mid-wall, usually in the areas where the wall is the thickest -insertion points of the septum to the RV level | -increased | -increased | -normal -slightly increased in the burnout type |
| ARVC | -RV dilatation, dysfunction, -akinetic, dyskinetic aneurysms at the RV level, often affecting the RV triangle: sub tricuspid area, RV ejection tract, and RV apex -LV systolic dysfunction, regional wall motion abnormality | - transmural RV region(s) (inlet, outlet, and apex) - subepicardial or mid-wall at LV lateral/inferolateral, septum, or both -subepicardial circumferential infiltration in those with predominantly LV damage | -decreased in fat infiltration -increased in scar region | -non-specific | - can be increased at the level of LGE in acute phases |
| Cardiac amyloidosis | -concentric hypertrophy -IAS, LA wall thickening - LV dysfunction -pericardial effusion | -diffuse subendocardial -nulling effect of the myocardium -dark blood aspect | -diffuse increased | -very increased | -non-specific pattern - can be increased in those with AL form |
| Cardiac sarcoidosis | -global systolic dysfunction -regional or global wall motion abnormalities, -bi-ventricular dilatation or hypertrophy. -slight increase in left ventricular mass secondary to granulomatous expansion | -mid-wall or sub-epicardial focal fibrosis, -transmural or subendocardial, but without a correlation to a coronary territory -papillary muscles, RV-free wall, and the atria can also be involved. | -increased in the scar zone | - increased diffuse | -increased in areas with granulomas |
| LV non-compaction/hypertrabeculation | -noncompacted-to-compacted myocardium ratio of 2.3:1 -trabeculated mass > 20% - LV disfunction/dilatation | -non-specific pattern -most frecvent subepicardial | -slightly increase | -increased diffuse | -normal |
| Anderson-Fabry disease | -concentric important LV hypertrophy | -mid-wall inferolateral -mid-wall septal | -decreased - pseudonormal | -decreased | -slightly increased, basal anteroseptal |
| Neuromuscular dystrophy | -normal -LV dysfunction -regional wall motion defects | -focal fibrosis predominantly at the level of the lateral and inferolateral walls | -increased diffuse | -increased diffuse | -hypersignal at the LGE level |
CMR parameters_ Predictor of significant clinical impact-univariable analysis
| Predictor | N | Event N | OR (95% CI)1 | p-value |
|---|---|---|---|---|
| LVEF | 272 | 180 | 0.97 (0.95 to 0.99) | 0.002 |
| LVEDVi | 272 | 180 | 1.01 (1.00 to 1.01) | 0.067 |
| LVESVi | 272 | 180 | 1.01 (1.00 to 1.02) | 0.012 |
| LVSVi | 272 | 180 | 0.98 (0.96 to 1.00) | 0.026 |
| RVEF | 265 | 175 | 0.97 (0.95 to 0.99) | 0.002 |
| LGE | 177 | 113 | 1.84 (1.11 to 3.07) | 0.019 |
| Native septal T1 | 243 | 157 | 1.00 (1.00 to 1.01) | 0.507 |
| T2 | 254 | 167 | 0.99 (0.93 to 1.01) | 0.387 |
Demographic Parameters_ Predictor of significant clinical impact - univariable analysis
| Predictor | N | Event N | OR (95% CI)1 | p-value |
|---|---|---|---|---|
| Age | 272 | 180 | 1.00 (0.99 to 1.02) | 0.733 |
| Gender (M) | 179 | 121 | 1.20 (0.71 to 2.03) | 0.492 |
| BSA | 272 | 180 | 1.22 (0.53 to 2.96) | 0.643 |
| Coronary angiography | 57 | 41 | 1.39 (0.74 to 2.71) | 0.312 |
| Hypertension | 151 | 102 | 1.16 (0.70 to 1.93) | 0.559 |
| Hypercholesterolemia | 140 | 95 | 1.18 (0.71 to 1.96) | 0.517 |
| Alcohol | 12 | 10 | 2.66 (0.68 to 17.6) | 0.212 |
| Tabacco use | 40 | 28 | 1.24 (0.61 to 2.64) | 0.568 |
| NYHA class | ||||
| 1 | 29 | 19 | — | |
| 2 | 176 | 110 | 0.88 (0.37 to 1.96) | 0.755 |
| 3 & 4 | 36 | 29 | 2.18 (0.72 to 6.97) | 0.175 |
CMR parameters
| Cardiac dimensions and function | |
|---|---|
| LVEDV, ml | 224 (±100) |
| LVEDVi, ml/m2 | 113(± 47) |
| LVESV, ml | 129 (±92) |
| LVESVi, ml/m2 | 64 (±43) |
| LVSV | 92 (±58) |
| LVEF, % | 46 (±15) |
| LV mass i, g/m2 | 68(±27) |
| RVEDV, ml | 168 (±58) |
| RVEDVi, ml/m2 | 81 (±29) |
| RVESV, ml | 89 (±27) |
| RVESVi, ml/m2 | 43 (±26) |
| RVEF% | 55 (±11) |
| Tissue characterization | |
| Oedema n, (%) | 15, (4,2%) |
| Native T1 (ms) | 1030(±50) |
| T2 (ms) | 49 (±19) |
| Characterization of focal scars | |
| Scar present n, (%) | 177 (65%) |
| Non-ischaemic scar n, (%) | 164 (92%) |
| Ischaemic scar n, (%) | 13 (7.3%) |
Number of scars (%)
|
|
Baseline characteristics
| Baseline characteristics | |
| Age, years | 49 (±14) |
| Sex (male), % | 65% |
| Body surface area, m2 | 1.99 (±0.2) |
| Family history of cardiomyopathy | 4% |
| NYHA Class | |
| I | 21% |
| II | 65% |
| III | 13% |
| IV | 1% |
| Coronary artery risk factors | |
| Hypertension, % | 55% |
| Diabetes mellitus, % | 3% |
| Hypercholesterolemia, % | 51% |
| Smoking % | 15% |
| Alcohol consumption, % | 4.5% |
| Comorbidities | |
| History of myocardial infarction, % | 0.5% |
| Aortocoronary bypass operation, % | 0% |
| PCI, % | 0.5% |
| CKD, % | 5% |
| Electrocardiogram | |
| Sinus Rhythm, % | 93% |
| Atrial Fibrillation, % | 7% |
| Complete LBBB, % | 12% |
| Frequent PVC, % | 7% |
| Complications | 0.5% |
| Cardiac tests before CMR | |
| Echocardiography | 100% |
| Coronary angiogram CT | 1% |
| Coronary angiography | 20% |
| SPECT | 1% |
| Treadmill test | 2% |
| The primary indication for CMR | |
| DCM/ NDLVC | 45% |
| HCM/ LVH | 18% |
| Cardiac amyloidosis | 5.2% |
| ARVC | 4 % |
| Myocarditis | 3.6% |
| Cardiac sarcoidosis | 1% |
| LV non-compaction/hypertrabeculation | 2% |
| Anderson-Fabry disease | 2% |
| Tachycardia-induced cardiomyopathy | 1% |
| Chemotherapy induces cardiomyopathy | 0.5% |
| Neuromuscular cardiomyopathy | 0.5% |
| Arrhythmia/SND substrate | 2.5% |
| Ischemic cardiomyopathy | 1% |
| Other cardiomyopathy | 10% |
CMR parameters_ Multiple univariate binominal logistic regression
| Predictor | N | SCI N | OR (95% CI) 1 | p-value | VIF1 |
|---|---|---|---|---|---|
| LVESVi | 272 | 180 | 1.01 (1.005 to 1.02) | 0.021 | 1.0 |
| LGE | 177 | 113 | 1.72 (1.03 to 2.89) | 0.038 |